Caring for the feet of diabetics
Updated on , validated by the medical directorate.
Both type 1 and type 2 diabetes can cause skin symptoms and conditions. The feet of diabetics are not spared¹. What happens to the skin in diabetics? And, in particular, the feet? What are the causes? What are the complications? How do you take care of your feet when you have diabetes?
- 82
of diabetic patients suffer from xerosis of the foot1
- 3x more
foot lesions in a diabetic patient2
- https://medlineplus.gov/diabeticfoot.html
- A Lechner, M Akdeniz et al. : Comparing skin characteristics and molecular markers of xerotic foot skin between diabetic and non-diabetic subjects: An exploratory study; Journal of Tissue Viability; 28(4): 200-209

Summary
Xerosis in diabetics
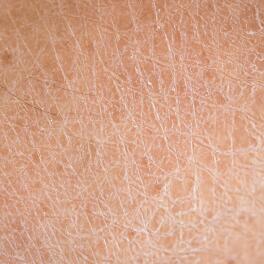
Skin disorders are common in patients with type 1 and 2 diabetes2. People with high blood sugar levels have 1.5 times more skin problems than those with normal blood sugar levels3. Among the most common problems is diabetic xerosis,4 which is defined as a dry skin condition5. The latter is partly explained by a decrease in the functioning of the glands that produce sweat. This makes the skin drier and more fragile6. Xerosis is the earliest and most common manifestation of diabetes and will mainly affect the shin area and the feet7,8.
Failure to diagnose and treat skin disorders, including xerosis, at an early stage can lead to the development of open cracks or fissures, which are susceptible to infections, particularly bacterial and fungal2.
Foot problems are common in diabetic patients. They occur over time, especially when hyperglycaemia is not adequately controlled9. Xerosis of the foot, with or without cracks or fissures, is observed in 82% of diabetic patients9. In addition, one study showed that the skin of a diabetic patient has, on average, three times more lesions on the feet than a non-diabetic patient10.
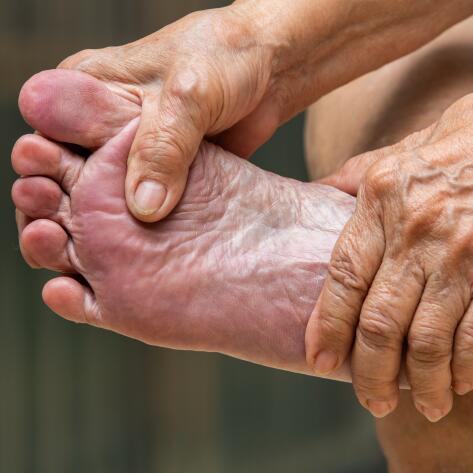
Beyond the problem of xerosis, hyperglycaemia as a result of diabetes has other physiological consequences11,12:
- Diabetic neuropathy, which is an injury to the nerve fibres. When sensory nerves are affected, i.e. those that transmit sensory information such as touch, heat or pain, there is a decrease in sensitivity. This symptom starts in the feet and then gradually moves upwards. This means that pain can no longer play its role as a warning and the risk of a wound that can become superinfected is increased.
- Diabetic arteriopathy, which is a disease of the arteries. Hyperglycaemia encourages cholesterol deposits on the artery walls, which are known as atheromatous plaques. This reduces the diameter of the arteries and, therefore, blood flow. Lower limb arteriopathy occurs when the legs are affected. The blood supply to the feet decreases and this increases the risk of ulceration, decreases healing and reduces the influx of white blood cells involved in the immune response to fight off possible infections.
The combination of dry skin, loss of sensitivity and poor circulation increases the risk of foot infections in diabetics. The main complication that can be observed is called diabetic foot. It is defined as destruction of the foot tissue13. If left untreated, the wound can become infected with micro-organisms, have difficulty healing and can end in amputation if gangrene occurs. It is estimated that 10% of diabetics are at risk of amputation.
It is also believed that the majority of these amputations could be avoided, mainly through better prevention and more suitable daily care6.
How do you minimise the risk of foot infections in diabetics?
Fortunately, the management of diabetes has improved considerably and current treatments allow patients to better manage their disease. The number of amputations due to diabetes has decreased significantly14.
In addition to sticking to dietary rules and diabetes treatments, it is essential for diabetics to pay special attention to their feet every day. Simple habits can be implemented to limit the risk of infection15:
- Wash feet daily with a mild soap. Dry them meticulously, concentrating on the space between the toes. Avoiding soaking the feet for more than 10 minutes and avoiding water that is too hot are both recommended.
- Combat xerosis by moisturising at least once a day with a suitable cream. This will prevent or reduce the formation of calluses and cracks that can be the gateway to superinfection.
- Nails should also be well maintained. Use a nail file rather than scissors or nail clippers to prevent injury. Nails should not be shorter than the tip of the toe, so that they can fulfil their protective role in case of impact.
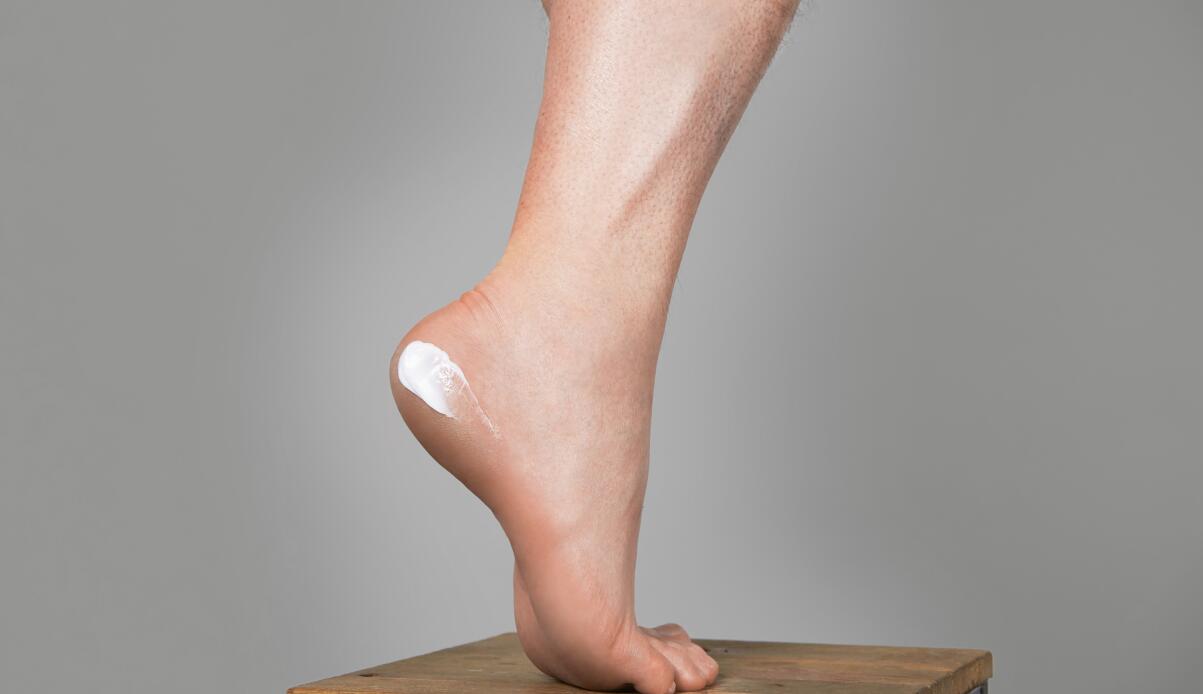
- Corns and calluses should be carefully monitored and treated gently. If in doubt, consult a pedicurist.
- Preferably wear cotton socks or socks made of a soft material that avoids maceration and rubbing. If there are any circulatory problems, opt for compression socks or stockings.
- Change your choice of shoes: they should be closed to protect the forefoot as much as possible, wide at the toe and without seams in the sensitive areas of the foot. There are specific shoe ranges for diabetics.
- It is important to examine your feet daily, even if there are no symptoms. This ensures that there is no wound (even a small one), no fungus, no blister or anything else.
- Finally, diabetics should have their feet examined at least once a year by a doctor. In addition to looking for wounds, the doctor will carry out a check-up and assess the sensitivity of the feet and legs, reflexes and muscle strength.
If in doubt, consult a doctor as soon as possible to detect any hidden complications11.
OUR MAIN RECOMMENDATIONS TO PREVENT THE RISK OF FOOT INFECTIONS IN DIABETICS
Moisturise your skin once a day
File your nails regularly
Are you aware of the effectiveness of DEXERYL Emollient Cream in the management of your condition?
DEXERYL Emollient Cream provides patients with proven clinical studies.
DEXERYL Emollient Cream: a partner of choice for diabetic foot care
Meticulous hygiene and care of the feet of diabetics is essential to avoid the risk of infection and complications.

DEXERYL Emollient Cream
Dexeryl Emollient Cream can be used to protect the skin and treat the signs and symptoms of dry skin, particularly the dry skin of diabetic patients.

Dexeryl supports you each day
Sources:
- https://diabetes.org/diabetes/foot-complications
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5006568/
- Campos de Macedo, G. M. C., Nunes, S., & Barreto, T. (2016). Skin disorders in diabetes mellitus: an epidemiology and physiopathology review. Diabetology & Metabolic Syndrome, 8(1). https://doi.org/10.1186/s13098-016-0176-y
- N Chatterjee, C Chattopadhyay et al. : An observational study of cutaneous manifestations in diabetes mellitus in a tertiary care hospital of Eastern India. Indian J Endocrinol Metab. 2014; 18: 217–220. doi: 10.4103/2230-8210.129115.
- https://www.larousse.fr/encyclopedie/medical/xérose/17061
- Bristow I (2013) Emollients in the care of the diabetic foot. The Diabetic Foot Journal 16: 63-6
- Pavlovic MD, Milenkovic T, Dinic M, Misovic M, Dakovic D, Todorovic S, et al. The prevalence of cutaneous manifestations in young patients with type 1 diabetes. Diabetes Care. 2007; 30: 1964-7
- Kirsner RS, Yosipovitch G, Hu S, Andriessen A, Hanft JR, Kim PJ, Lavery L, Meneghini L, Ruotsi LC. Diabetic Skin Changes Can Benefit from Moisturizer and Cleanser Use: A Review. J Drugs Dermatol. 2019 Dec 1; 18(12): 1211-1217. PMID: 31860208
- https://medlineplus.gov/diabeticfoot.html
- A Lechner, M Akdeniz et al. : Comparing skin characteristics and molecular markers of xerotic foot skin between diabetic and non-diabetic subjects: An exploratory study; Journal of Tissue Viability; 28(4): 200-209
- https://www.ameli.fr/assure/sante/themes/diabete/diabete-symptomes-evolution/complications-pieds
- http://www.omedit-centre.fr/portail/gallery_files/site/136/2953/4197/4829/4830/4844.pdf
- https://www.revmed.ch/revue-medicale-suisse/2015/revue-medicale-suisse-477/pied-diabetique-infecte-du-diagnostic-a-la-prise-en-charge
- https://www.diabete.qc.ca/fr/vivre-avec-le-diabete/soins-et-traitements/soins-du-corps/le-diabete-et-le-soin-des-pieds
- J. Martini, C. Huertas et al. : Efficacy of an emollient cream in the treatment of xerosis in diabetic foot: a double-blind, randomized, vehicle=controlled clinical trial; JEADV 2017, 31, 743-747