Learn how to identify and treat eczema spots. Practical advice for prevention and care and when to consult a dermatologist.
Summary

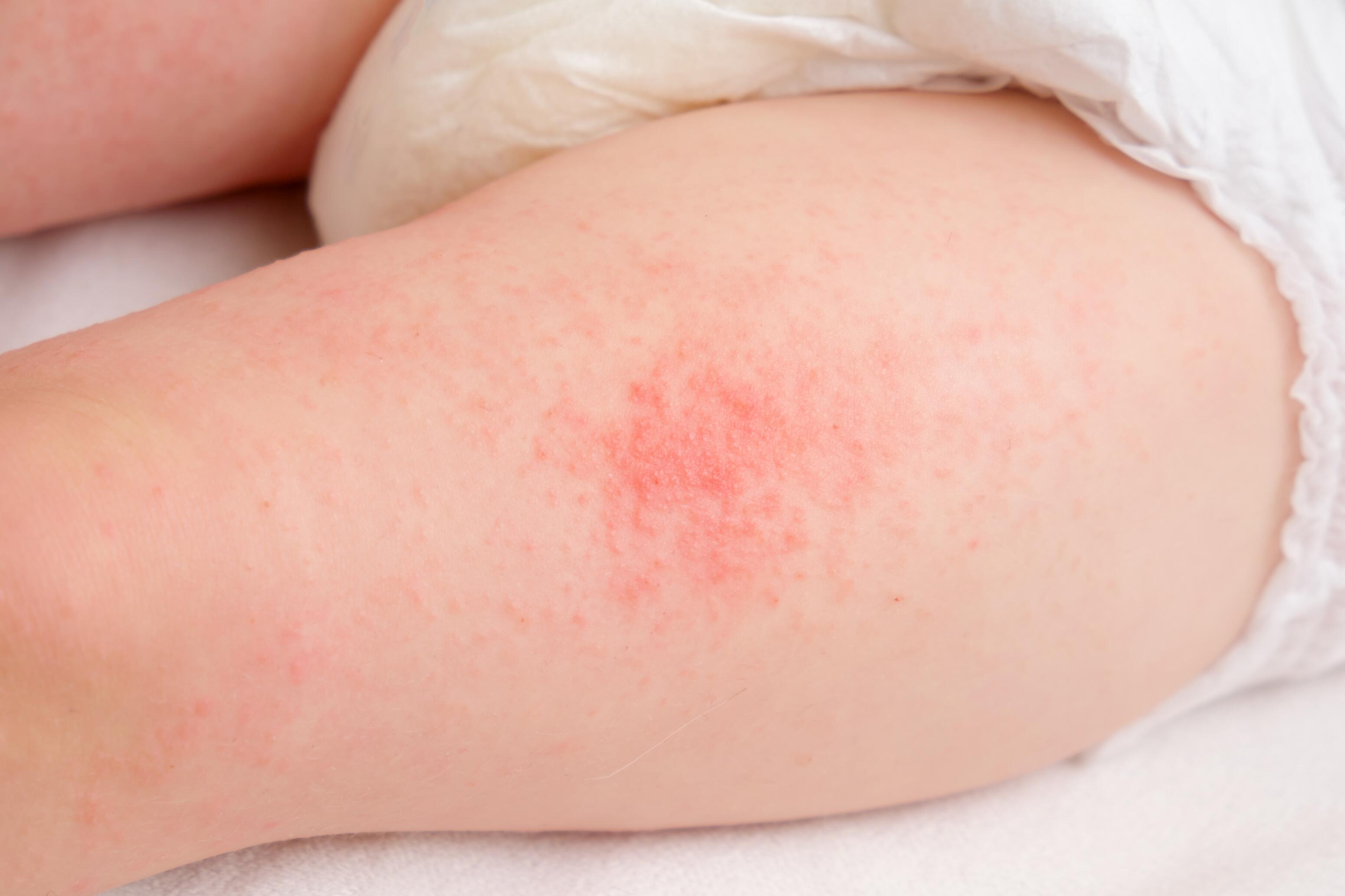
The term "spots" of eczema is somewhat misleading; eczema typically manifests as inflammatory patches, not spots in the same sense as the typical lesions of infectious diseases like measles or roseola.
The diagnosis of eczema is based on a clinical examination: eczema “spots” usually form red, often dry patches. On the surface of these patches, one can commonly find fine vesicles (collections of fluid with a diameter of less than 1 cm) that may break, causing oozing and crusting.
Significant itching usually accompanies eczema patches and may be associated with scratching lesions (excoriations), posing a risk of superinfection. Apart from the patches, the skin is generally dry, rough, and sometimes scaly. Over time, eczema-affected skin may change colour, become hypo- or hyperpigmented, and thicken, particularly in adults; this is referred to as lichenification.

Acne spots typically appear as papules (small raised lesions), vesicles, or pustules (raised lesions containing pus) and may be accompanied by blackheads or whiteheads (comedones), cysts, or even nodules (deep lesions extending into the dermis). Compared to eczema, acne lesions are oilier and often on the face, back, and chest.
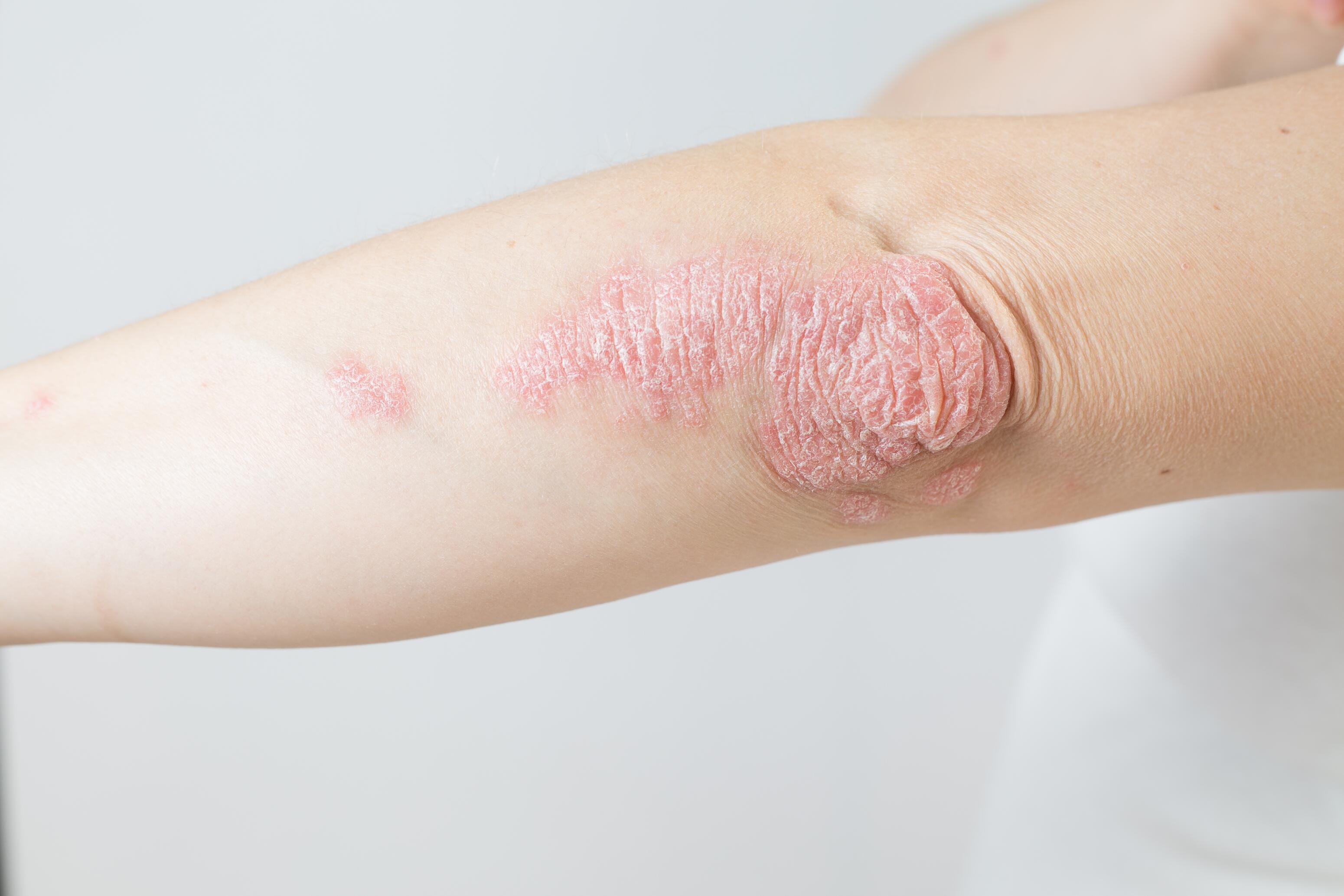
Eczema differs from psoriasis’ thick, well-defined patches covered in silvery scales. These patches are often located on the elbows, knees, and scalp. Eczema presents less thick lesions, with more pronounced redness and inflammation, skin dryness, and oozing.
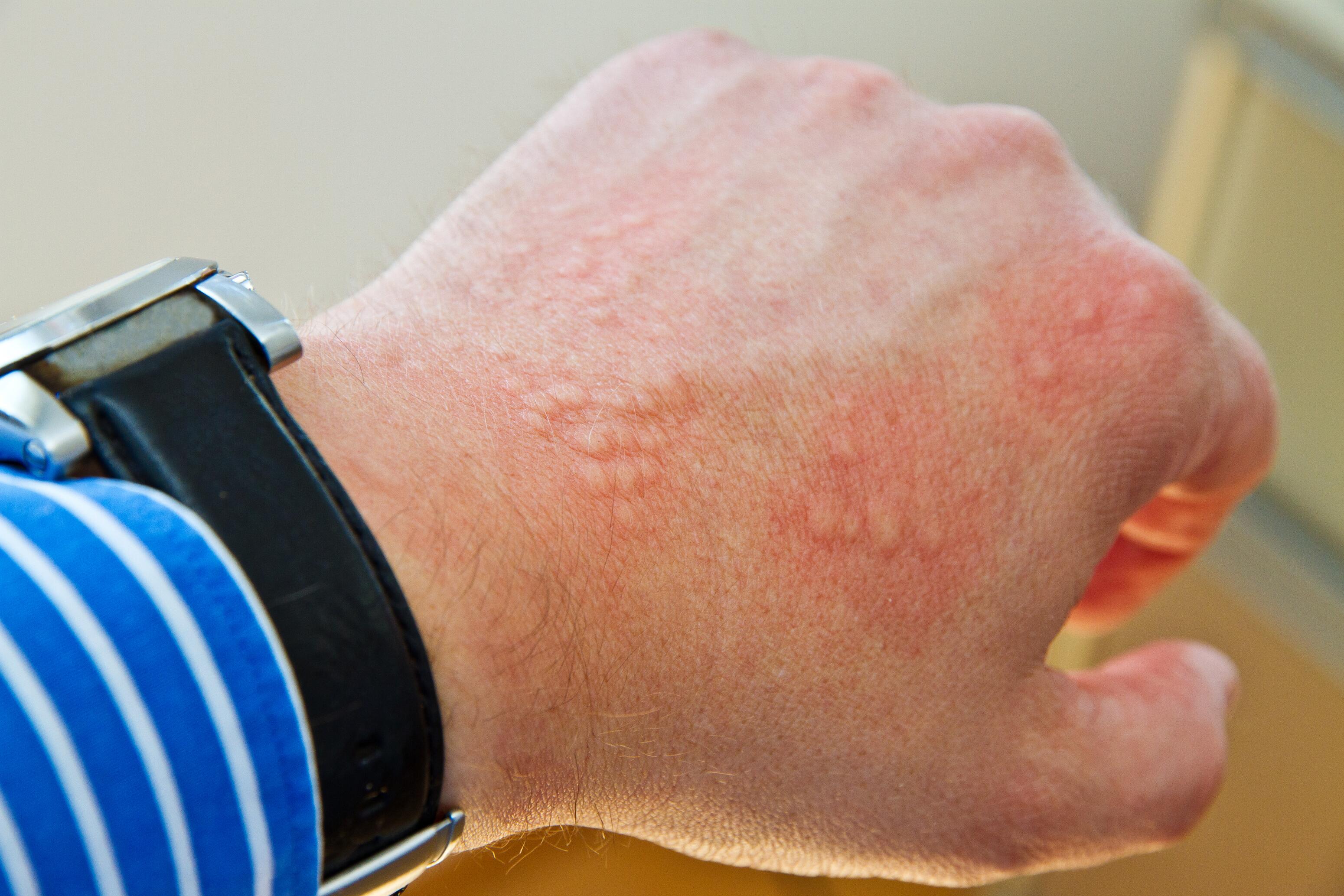
Urticaria symptoms manifest as papules or redness in swollen patches resulting from local oedema. These lesions, resembling nettle stings, are usually temporary and often disappear within less than 24 hours. Eczema, on the other hand, presents persistent patches that can last several days or weeks.
Scabies is a skin disease caused by a mite that induces intense itching, especially at night. Typical lesions include burrows and papules, particularly between the fingers, on the wrists, and around the waist.


Fungal skin infections, such as dermatophytes, manifest as patches and redness that preferentially affect folds (groins, spaces between the toes). Outside of folds, they can take on a characteristic ring-shaped appearance.
The causes of eczema are multifactorial, involving genetic, immune, and environmental factors.

Multiple genetic mutations, notably in a skin protein gene called filaggrin, contribute to skin dryness in atopic dermatitis. If parents have a history of eczema or other non-cutaneous allergies such as asthma or allergic rhinitis, their child is at a higher risk of developing eczema.
In individuals with eczema, atopic dermatitis especially, the immune system overreacts to normally harmless substances, leading to skin inflammation and eczema patches.

The most common triggers for eczema patches include:
- Climate (cold and dry weather or, conversely, excessive humidity).
- Environmental allergens (mites, dust, pollens) and pollutants (urban pollution, tobacco smoke).
- Food allergens (eggs, milk, peanuts), especially in infantile atopic dermatitis.
- Lifestyle and hygiene habits (too frequent showers, harsh soaps or drying).
- Stress.
- Irritants and chemicals (synthetic fabrics, soaps, detergents) are particularly at risk of contact eczema.
To treat eczema patches, dermatologists prescribe topical corticosteroids in creams or ointments. These reduce inflammation and itching.
Thus, inflammatory areas should be treated with topical corticosteroids once a day, preferably in the evening, extending beyond the lesions.
In more severe cases, topical immunomodulators (tacrolimus or pimecrolimus ointment) or systemic treatments (phototherapy, immunosuppressants, monoclonal antibodies) can better control flare-ups.
It's crucial to meticulously follow the doctor's instructions for applying topical corticosteroids in terms of frequency and duration of use.
During flare-ups, emollients should not be applied to inflammatory lesions. However, if the skin is dry, they can be applied to the rest of the body.
A gentle skincare routine is recommended daily to prevent eczema flare-ups. It's now recommended not to take a daily bath or shower but to space them out, except in case of sweating from effort or during summer. Use lukewarm water and a mild cleanser, and then dry gently without rubbing.
After bathing or showering, apply a hypoallergenic emollient when the skin is still slightly damp to maximise effectiveness.
Favour cotton clothing and ensure your clothes are thoroughly rinsed after washing to remove any detergent residue. Avoid wool garments, synthetic fabrics, and fragranced fabric softeners that can cause skin irritation.
In your home environment, maintain a cool temperature and ventilate often to reduce allergens and irritants. Keep your nails short to avoid scratching lesions and related complications.
Quitting smoking is beneficial in terms of lifestyle. Exercise and avoiding activities that cause excessive sweating are recommended. Take a shower after exercising and apply an emollient. Reinforce the application of emollients when the weather is cold and dry. Finally, do not change your diet without medical consultation unless a specific food allergen is identified.
Skin hydration is central in preventing eczema flare-ups. Emollients, applied twice daily every day to the entire body:
- Prevent skin dryness.
- Strengthen the skin barrier.
- Reduce the risk of flare-ups.
- Help relieve itching.
- Reduce the need for topical corticosteroid treatments.
Applying emollients after bathing or showering maximizes their effectiveness when the skin is still slightly damp. To minimize the risk of allergy, it's also beneficial to include in your skincare routine products specifically formulated for sensitive and eczema-prone skin.
It's crucial to consult a dermatologist if you notice a worsening of eczema symptoms, such as increased itching, spreading spots and lesions, oozing, bleeding, and signs of infection (painful spots, changing appearance, fever). A dermatologist can also intervene in cases of diagnostic doubt, side effects from treatments, or if eczema impacts your quality of life (stress, sleep disorders, impact on social or professional life).
If usual eczema treatments become less effective or flare-ups become more frequent or severe, this may indicate a disease progression that requires reevaluation. Furthermore, unusual symptoms like pain, excessive heat at the lesion sites, or sudden changes in the texture or colour of the skin should also prompt a consultation.
A dermatologist can provide a personalized approach to managing eczema lesions, including adjusting ongoing treatments, prescribing more suitable medications, and advising on skincare and preventive measures. Regular consultations are also recommended for optimal follow-up, particularly in adults and chronic or severe eczema cases. The dermatologist can also assess treatment effectiveness, detect potential complications or errors in treatment management, and adapt the care and prevention strategy according to the disease's progression.
A dermatologist can provide a personalized approach to managing eczema lesions, including adjusting ongoing treatments, prescribing more suitable medications, and advising on skincare and preventive measures. Regular consultations are also recommended for optimal follow-up, particularly in adults and chronic or severe eczema cases. The dermatologist can also assess treatment effectiveness, detect potential complications or errors in treatment management, and adapt the care and prevention strategy according to the disease's progression.
Reference:
1. Nemeth V, Evans J. Eczema. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2023 Jan. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK538209/
2. L’Assurance Maladie. Eczéma ou dermatite atopique : causes, symptômes et évolution. Ameli.fr. 2023 Sep. [Disponible sur :] https://www.ameli.fr/assure/sante/themes/eczema-atopique/reconnaitre-eczema-atopique
3. Benedetti J. Description of Skin Lesions. MSD Manuals Professional Edition. 2022 Sep. [Disponible sur :] https://www.msdmanuals.com/professional/dermatologic-disorders/approach-to-the-dermatologic-patient/description-of-skin-lesions
4. Sutaria A, Masood A, Saleh H, Schlessinger J. Acne Vulgaris. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2022 Aug. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK459173/
5. Barrett M, Luu M. Differential Diagnosis of Atopic Dermatitis. Immunol Allergy Clin North Am. Février 2017.
6. L’Assurance Maladie. Urticaire : symptômes et causes. Ameli.fr. 2023 Oct. [Disponible sur :] https://www.ameli.fr/assure/sante/themes/urticaire/reconnaitre-urticaire
7. L’Assurance Maladie. La consultation et le traitement en cas d'eczéma ou dermatite atopique. Ameli.fr. 2023 Sep. [Disponible sur :] https://www.ameli.fr/assure/sante/themes/eczema-atopique/consultation-traitement
8.L’Assurance Maladie. Dermatite atopique : que faire et quand consulter ? Ameli.fr. 2023 Sep. [Disponible sur :] https://www.ameli.fr/assure/sante/themes/eczema-atopique/que-faire-quand-consulter