The Different Types of Eczema: How to Recognise Them?
Updated on ,validated by the medical directorate.
Explore the various types of eczema, their hallmark symptoms, and practical treatment solutions.
The Main Types of Eczema: Description, Symptoms, and Diagnosis

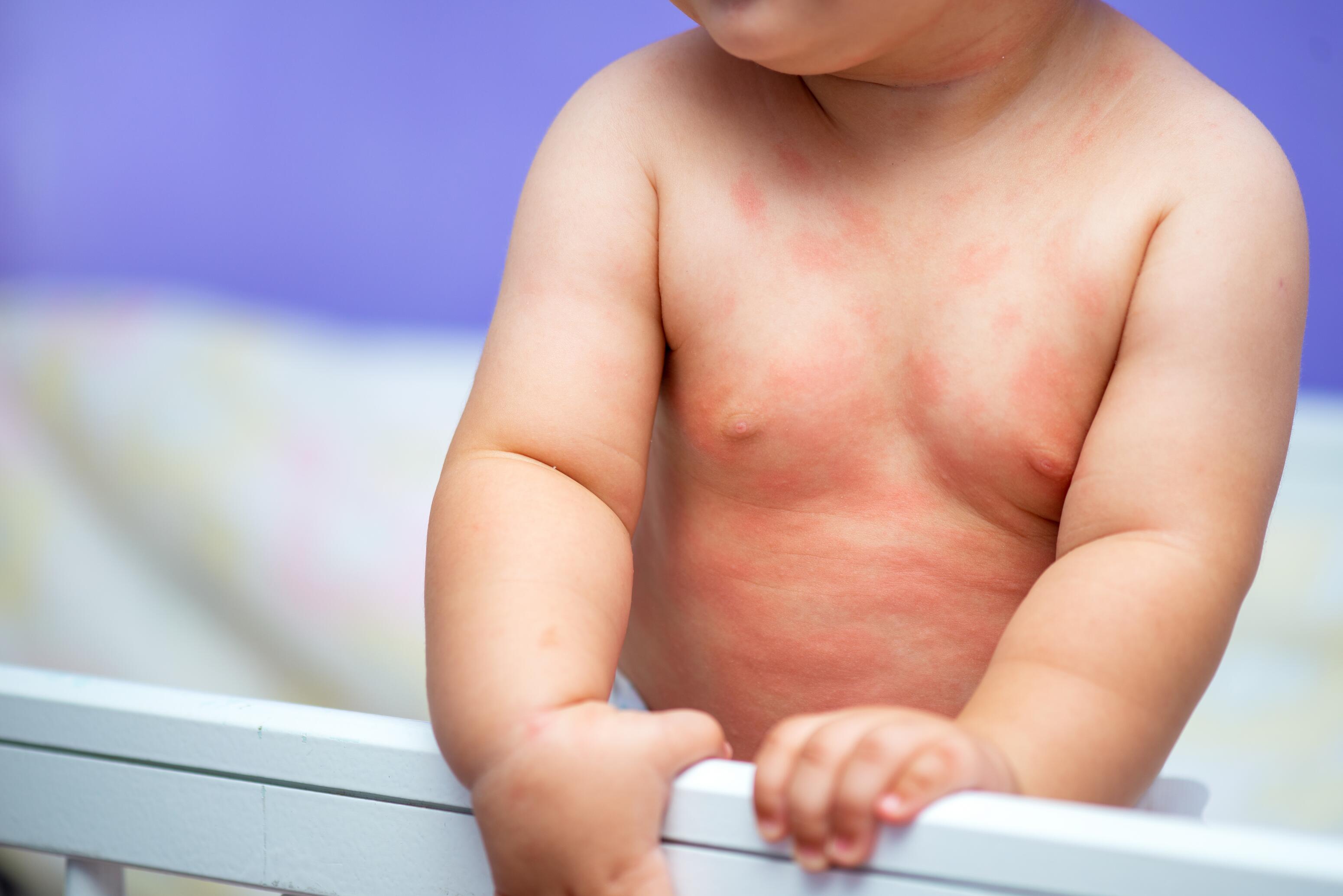
Atopic Eczema¹
The most common chronic inflammatory skin disease, atopic dermatitis, also known as atopic eczema, typically affects infants with a family history of atopy (eczema, asthma, allergic rhinitis). Its symptoms include skin dryness, itching, and lesions like red patches, blisters, oozing, and crusts. Atopic eczema typically cycles through flare-ups with symptom onset or exacerbation and remission phases with few or no symptoms.
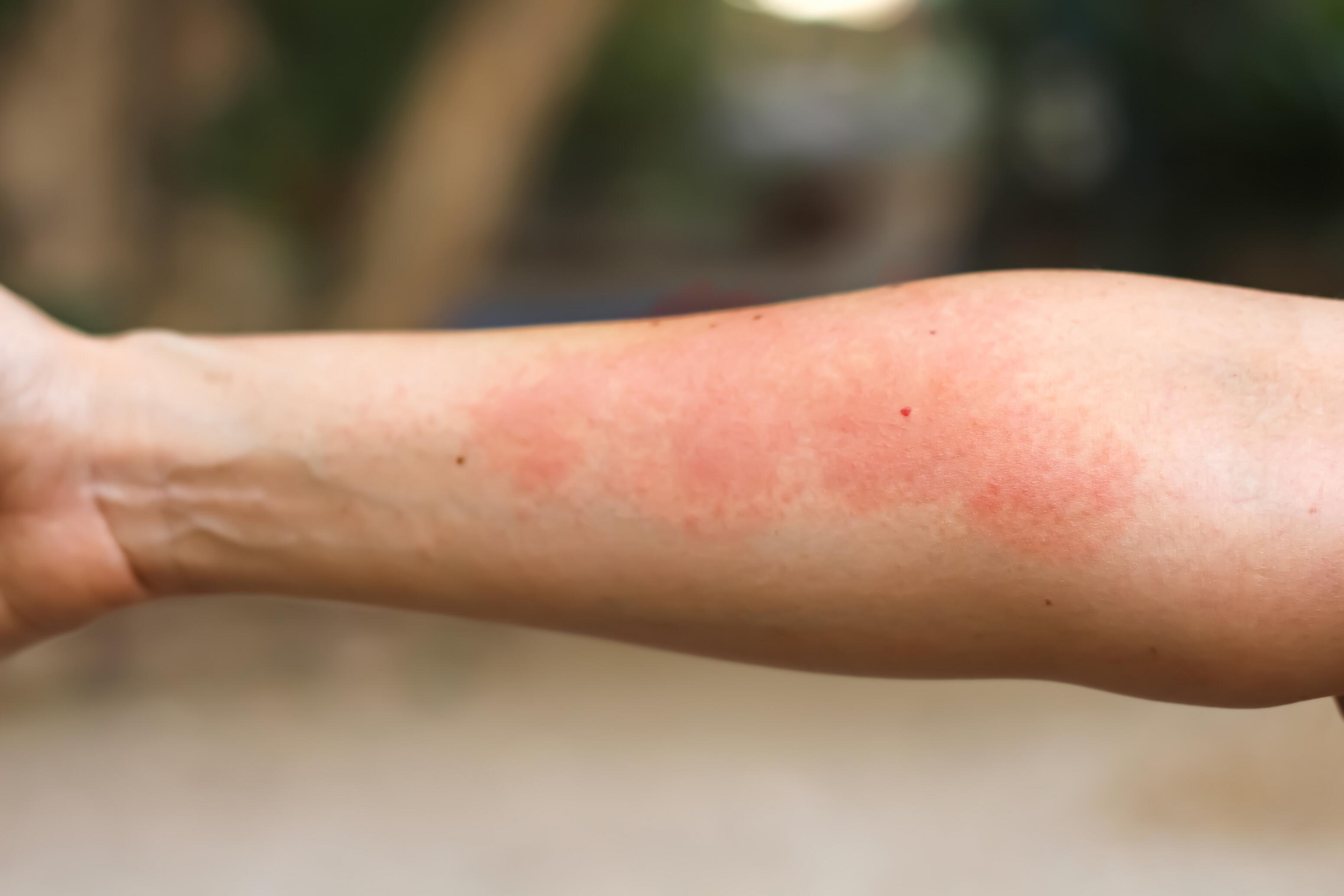
Contact Eczema²
There are two types of contact eczema: irritant and allergic. They occur directly on the affected areas when the skin comes into contact with an irritant or allergen (mainly the hands, neck, and face).
The diagnosis of contact dermatitis requires a consultation with a doctor (considering occupation, hobbies, use of topical treatments, etc.). Patch tests are the gold standard for identifying specific substances causing allergic contact eczema.

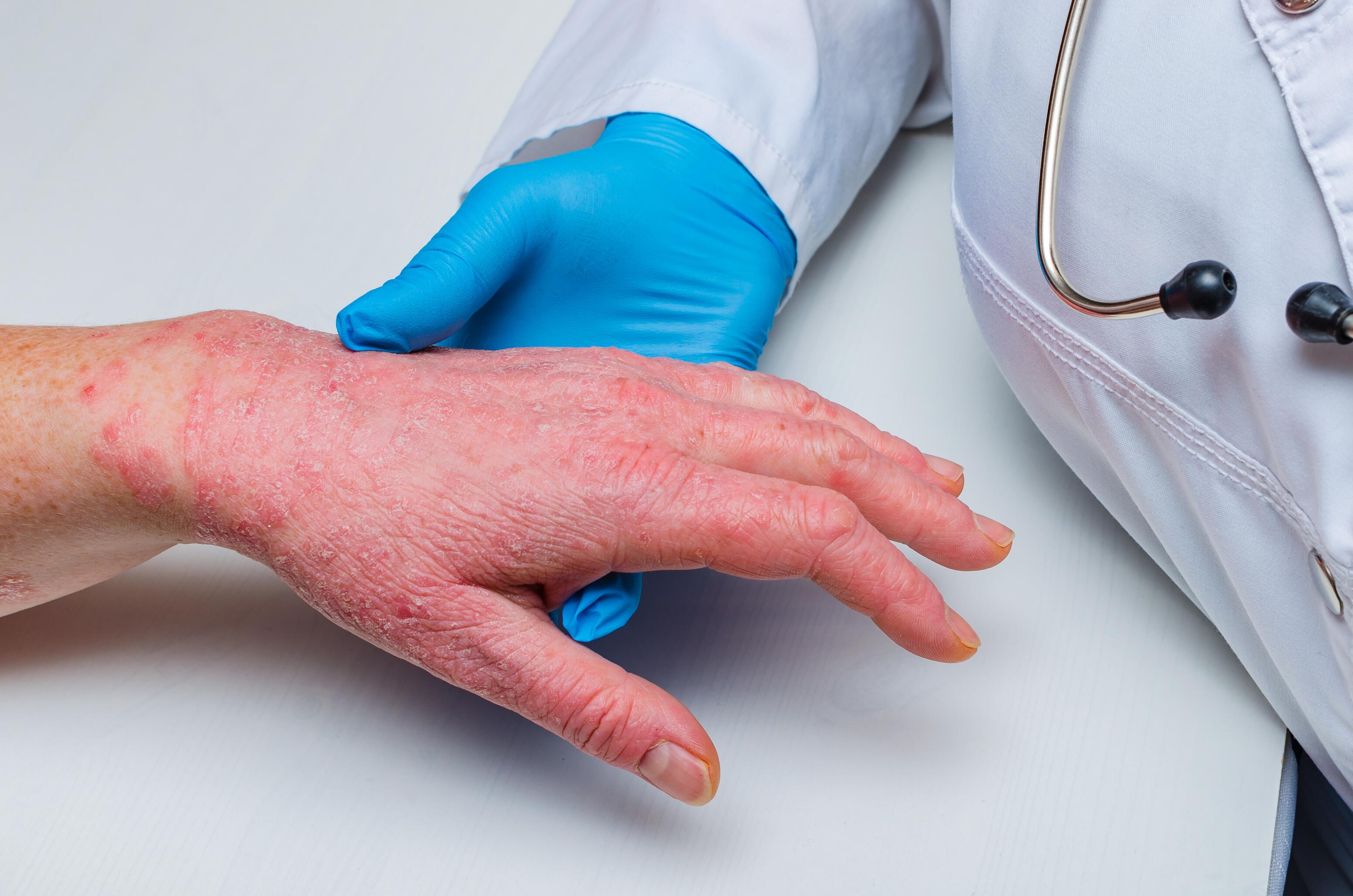
Chronic Hand Eczema³
Chronic hand eczema causes skin dryness, red patches, itching, burning sensations, deep, sometimes painful cracks, or even bleeding sores. It is a type of adult eczema, typically work-related.
Dyshidrosis⁴ ⁵
Dyshidrosis is a form of blistering eczema occurring in flare-ups. It is characterised by vesicles, possibly filled with fluid, on the palms of the hands and soles of the feet or the edges of the fingers and toes. It generally comes with intense itching, even burning sensations.

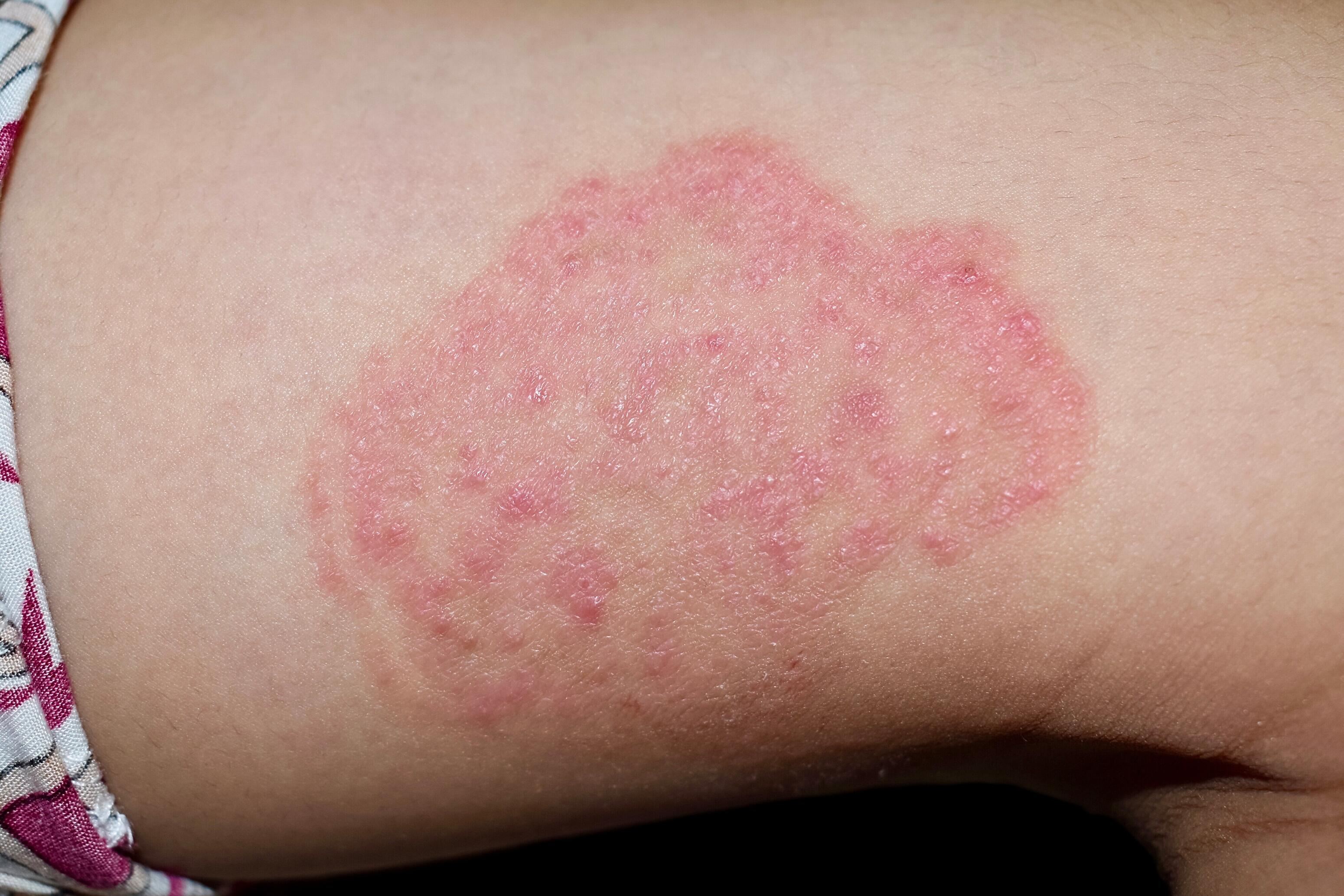
Nummular Eczema⁶
Nummular eczema is a type of chronic eczema characterized by coin-shaped lesions. These patches are generally found on the legs, arms, and hands. They are well-defined, sometimes oozing, and covered with crusts or scales.
Seborrheic Dermatitis⁷
This form of chronic eczema primarily affects areas of the skin rich in sebaceous glands like the scalp, face, and chest. The symptoms are red patches covered with dry scales that fall off as dandruff. These scales can also be oily and yellowish.

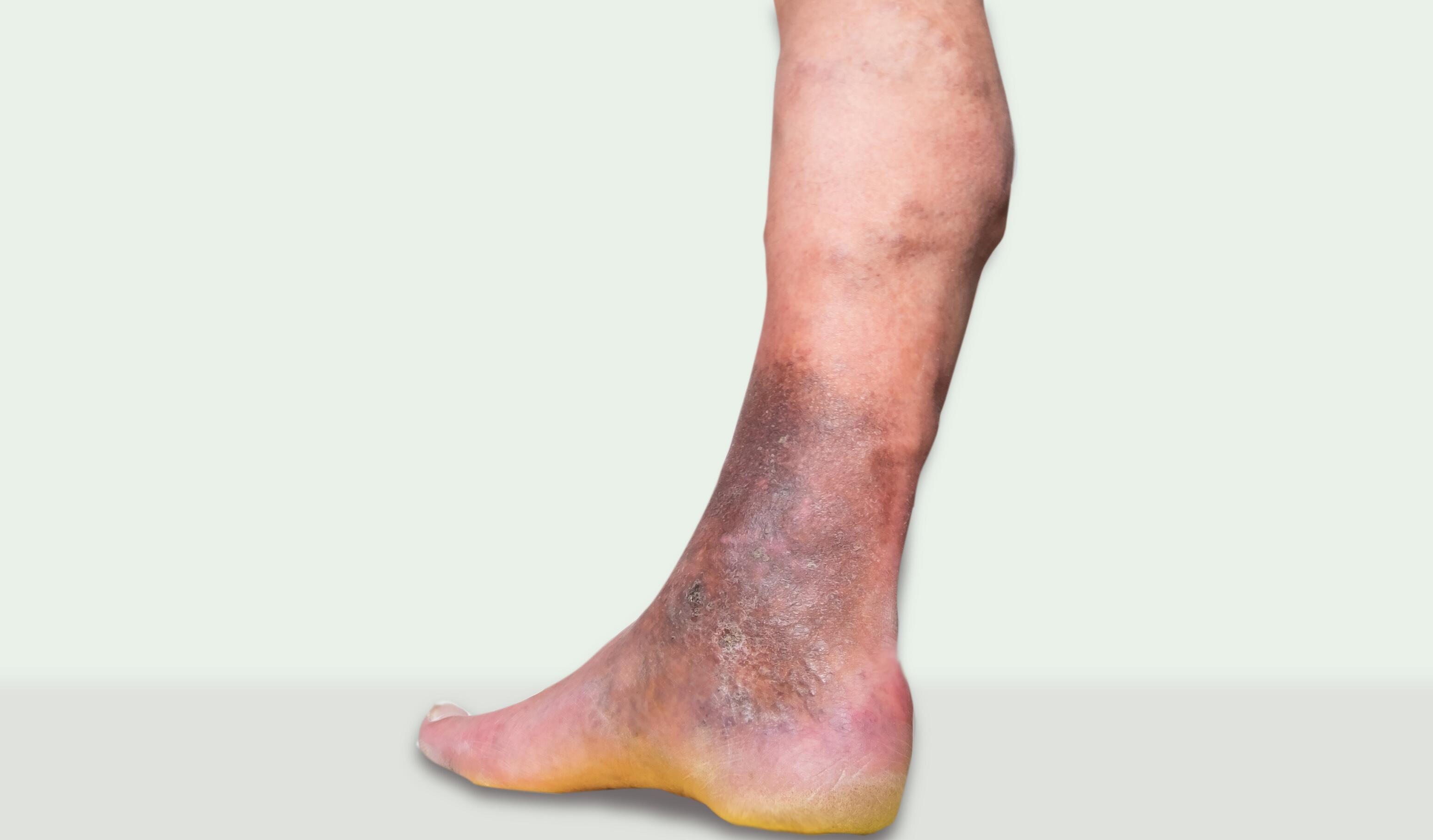
Varicose Eczema⁸
Also known as stasis dermatitis, this type of chronic eczema is due to venous disorders. The symptoms usually appear around the ankles or on the front of the legs: itching, redness, thickened and scaly skin, oozing, and ulceration.
In case of doubt, a doctor may prescribe a venous Doppler ultrasound.
What Causes the Different Types of Eczema?
Common Causes of All Eczemas¹ ⁹
The causes of eczema involve a complex interaction between several factors:
- The skin has structural abnormalities that prevent it from retaining water, leaving it porous to external aggressions.
- Environmental factors (climate, infections, etc.) trigger eczema symptoms.
Common Causes of Some Eczemas (excluding seborrheic and varicose eczema)¹ ⁹
Certain types of eczema may be favoured by:
- Genetic mutations, most often hereditary, affect the immune system and skin.
- The immune system is deregulated; it overreacts in an allergic manner.
- Psychological factors (stress) steer immunity towards an allergic response and disrupt the integrity of the epidermis.
Common causes of different types of eczema
Deregulated immune system
Skin permeable to external aggression
Psychological factors
Environmental factors
Causes and Triggering Factors Specific to Different Types of Eczema
Atopic Eczema¹
The triggering factors for atopic dermatitis, a genetic and environmental disease, vary from person to person. Among the most common are environmental allergens (pollens, moulds, dust mites), hypersensitivities and food allergies, irritants (soaps, tobacco), climate, and infections.
Contact Dermatitis²
Irritative contact dermatitis results from direct exposure to an irritant that damages the skin, such as:
- Chemicals: detergents, solvents, and acids.
- Soaps and cleansers.
- Frequent and prolonged exposure to water, especially hot water.
Allergic contact dermatitis is caused by an allergic reaction related to skin sensitisation to a specific substance, such as:
- Nickel (in jewellery and jean buttons).
- Fragrances and preservatives (cosmetics, lotions).
- Rubber (latex gloves).
- Glues and adhesives (bandages, craft products).
- Topical medications (active substances and excipients).
Chronic Hand Eczema³
Several factors exacerbate this type of chronic eczema: chemical irritants, water, cold and climate changes, repeated hand friction (e.g., chefs, nurses) and trauma, some medications, or skin infections.
Dyshidrosis⁴ ⁵
Its main triggering factors are chronic stress, excessive sweating, prolonged exposure to moisture, seasonal changes, fungal infections, and smoking.
Nummular Eczema⁶
The exact causes of nummular eczema are not fully understood, but several triggering factors have been identified: skin injuries, infections, climate, certain diseases (thyroid disorders), and treatments.
Seborrheic Dermatitis⁷
While its exact causes are not fully understood, this chronic disease is linked to excessive sebum production in areas rich in sebaceous glands. This excess sebum promotes the growth of Malassezia, a fungus naturally living on the skin, creating skin inflammation.
Its favouring factors include hormonal cycles, certain diseases (HIV, Parkinson's, depression, eating disorders), medications, inadequate personal hygiene, alcohol, and diet.
Varicose Eczema⁸
This eczema is most often associated with chronic venous insufficiency. Its risk factors are thus age, immobility, overweight, leg injuries and trauma, history of deep vein thrombosis, and skin infections.
Management and Prevention for Each Type of Eczema
Atopic Eczema¹
The prevention and treatment of atopic dermatitis involve:
- Regular use of emollients to moisturise the skin, strengthen its cohesion, and thus prevent flare-ups.
- Reducing triggering factors: avoiding allergens when possible, avoiding irritants, and preventing stress.
- Topical corticosteroids to reduce inflammation and itching.
- Exceptional treatments in some cases.
Contact Eczema²
The treatment of contact eczema primarily requires identifying and avoiding the substances involved. When this is not possible, wearing protective clothing is essential. Emollients are necessary to moisturise and restore the skin's integrity, and doctors may prescribe high-potency topical corticosteroids to reduce inflammation.
Chronic Hand Eczema³
Its treatment combines:
- Avoiding triggering factors when possible (including occupational reclassification).
- Protecting the skin by wearing gloves and appropriate clothing.
- Regular skin moisturisation with emollients.
- Topical medications (corticosteroids).
- Systemic treatments if needed.
Dyshidrosis⁴ ⁵
Treatments include the daily application of emollients to moisturise the skin and topical corticosteroids to reduce itching. A dermatologist may prescribe systemic treatments (oral corticosteroids, immunosuppressants, phototherapy) in severe cases.
Nummular Eczema⁶
Its treatment aims to restore the skin barrier by regularly applying emollients. Doctors may prescribe topical corticosteroids to reduce inflammation and itching.
Seborrheic Dermatitis⁷
Management is based on lifestyle changes (stress reduction, improved sleep, personal hygiene), skin moisturisation with emollients, antifungal medications (lotions and shampoos), and occasional topical corticosteroids.
Varicose Eczema⁸
Treatment involves managing venous insufficiency through venous compression. Applying emollients helps moisturise the skin, and topical corticosteroids reduce inflammation.
FAQ
The clinical signs of atopic dermatitis are dry, scaly skin, itching (or pruritus) and eczema-like red patches of skin. These are often located in the folds of the elbows, knees and neck. These lesions may ooze, form scabs and gradually thicken.
The difference between a healthy skin microbiome and that of atopic skin is the diversity and balance of bacteria. A healthy microbiome has a wide variety of beneficial bacteria, providing an effective protective barrier. By contrast, atopic skin often shows a reduction in this diversity, with an imbalance favouring pathogenic species. This imbalance can alter immune responses, making the skin more vulnerable to irritation and infection. In short, the composition of the microbiome influences skin health, differentiating balanced skin from atopic skin.
References
1. Kolb L, Ferrer-Bruker SJ. Atopic Dermatitis. National Library of Medicine. Treasure Island (FL): StatPearls Publishing; 2023 Jan. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK448071/
2. Litchman G, Nair PA, Atwater AR, et al. Contact Dermatitis. National Library of Medicine. Treasure Island (FL): StatPearls Publishing; 2023 Jan. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK459230/
3. Dubin C, Del Duca E, Guttman-Yassky E. Drugs for the Treatment of Chronic Hand Eczema: Successes and Key Challenges. Ther Clin Risk Manag. Décembre 2020;16:1319-1332.
4. Calle Sarmiento PM, Chango Azanza JJ. Dyshidrotic Eczema: A Common Cause of Palmar Dermatitis. Cureus. Octobre 2020;12(10):e10839.
5. Wollina U. Pompholyx: a review of clinical features, differential diagnosis, and management. Am J Clin Dermatol. 2010;11(5):305-14.
6. Robinson CA, Love LW, Farci F. Nummular Dermatitis. National Library of Medicine. Treasure Island (FL): StatPearls Publishing; 2022 Oct. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK565878/
7. Tucker D, Masood S. Seborrheic Dermatitis. National Library of Medicine. Treasure Island (FL): StatPearls Publishing; 2023 Jan. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK551707/
- Discover Causes of Eczema: Why Does It Occur and How Can You Prevent It?
Causes of Eczema: Why Does It Occur and How Can You Prevent It?
- Discover Eczema Symptoms: Identification and Understanding
Eczema Symptoms: Identification and Understanding