Uncover the essentials of hand and wrist dermatitis, from symptoms and underlying causes to effective treatments and daily care strategies

Summary
Hand dermatitis is a heterogeneous condition encompassing all eczemas localized on the hands and wrists, which have various causes, clinical forms, and durations [1]. This condition affects 9.1% of the general population [2].
As a chronic inflammatory skin disease, dermatitis can significantly impact daily life quality since its symptoms often disrupt manual activities and affect professional, social, and family life, sleep, and well-being [1,2].
Hand dermatitis is frequently triggered or worsened by occupational factors, often affecting individuals with professional activity or children [1].
By definition, acute hand dermatitis lasts less than three months and does not occur more than once a year, while chronic dermatitis lasts more than three months or occurs twice or more per year [1,2].
The symptoms of hand dermatitis vary according to the disease stage:
- In the acute stage, the skin may show redness, swelling, macules, papules, vesicles, oozing, and crusts.
- In the chronic phase, the main symptoms are scaling, hyperkeratosis (thickening of the outer layer of the skin), lichenification, and fissures.
These lesions are accompanied by subjective signs such as itching, burning sensations, pain, sleep disturbances, and mood disorders. Additionally, the aesthetic appearance of specific lesions (scales, hyperkeratosis, vesicles) can cause embarrassment or even lead to social or psychological difficulties.
The causes of hand and wrist dermatitis are multifactorial and complex.

The causes of hand dermatitis can be related to individual factors causing alterations in the skin barrier, making it permeable to allergenic and irritant factors and leading to abnormal immune reactions. Individuals with atopic dermatitis, especially those with filaggrin gene mutations, are likelier to develop hand dermatitis.
Environmental factors such as contact with water, working in a wet environment, and physical or chemical irritations can trigger or aggravate the symptoms of hand dermatitis. Cold and dry weather conditions, as well as low indoor humidity levels, are additional factors. Irritative contact dermatitis can promote allergic dermatitis by making the skin permeable to allergens.

The doctor must collect the medical history, look for personal and professional exposures, and examine the hands and the rest of the skin.
Patch tests, or epicutaneous tests, help to identify allergies and diagnose allergic contact eczema. Doctors perform them in the following cases:
These tests identify allergens in urticaria and protein contact dermatitis.
Sometimes, diagnosing hand dermatitis may require additional tests (infection screenings, skin biopsies).
Hand dermatitis's clinical forms and symptoms do not reflect the disease's causes. Hence, doctors use the causes of dermatitis and a description of the symptoms to classify it.
Several sub-diagnoses may be necessary to characterize the dermatitis. They can change over time.
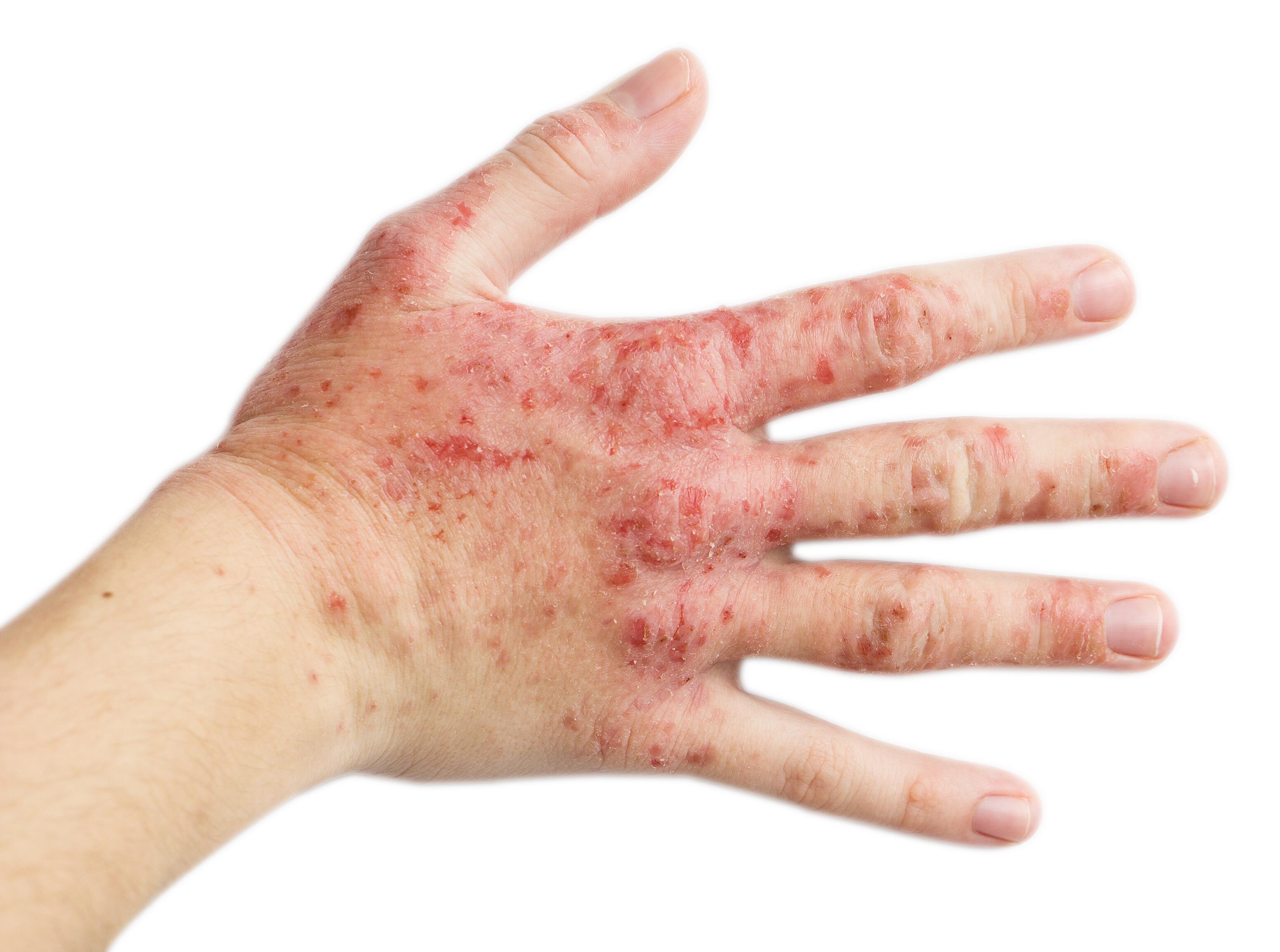
The most common form of hand dermatitis, irritative dermatitis, is associated with exposure to domestic or professional irritants. Symptoms are generally localized on the back of the fingers and hands.
This dermatitis is linked to exposure to allergenic factors. Symptoms of allergic dermatitis usually affect the fingertips or palms.
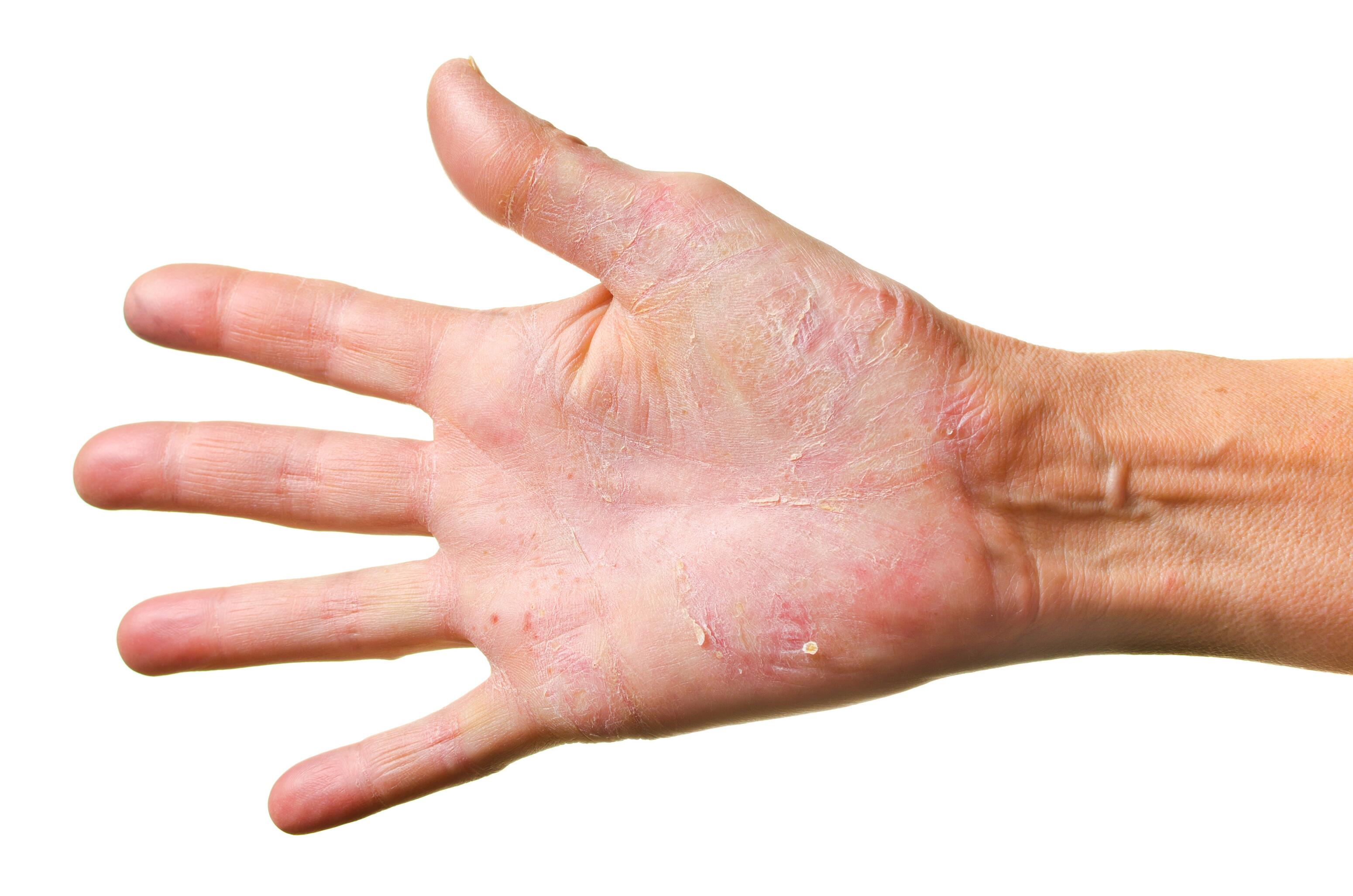
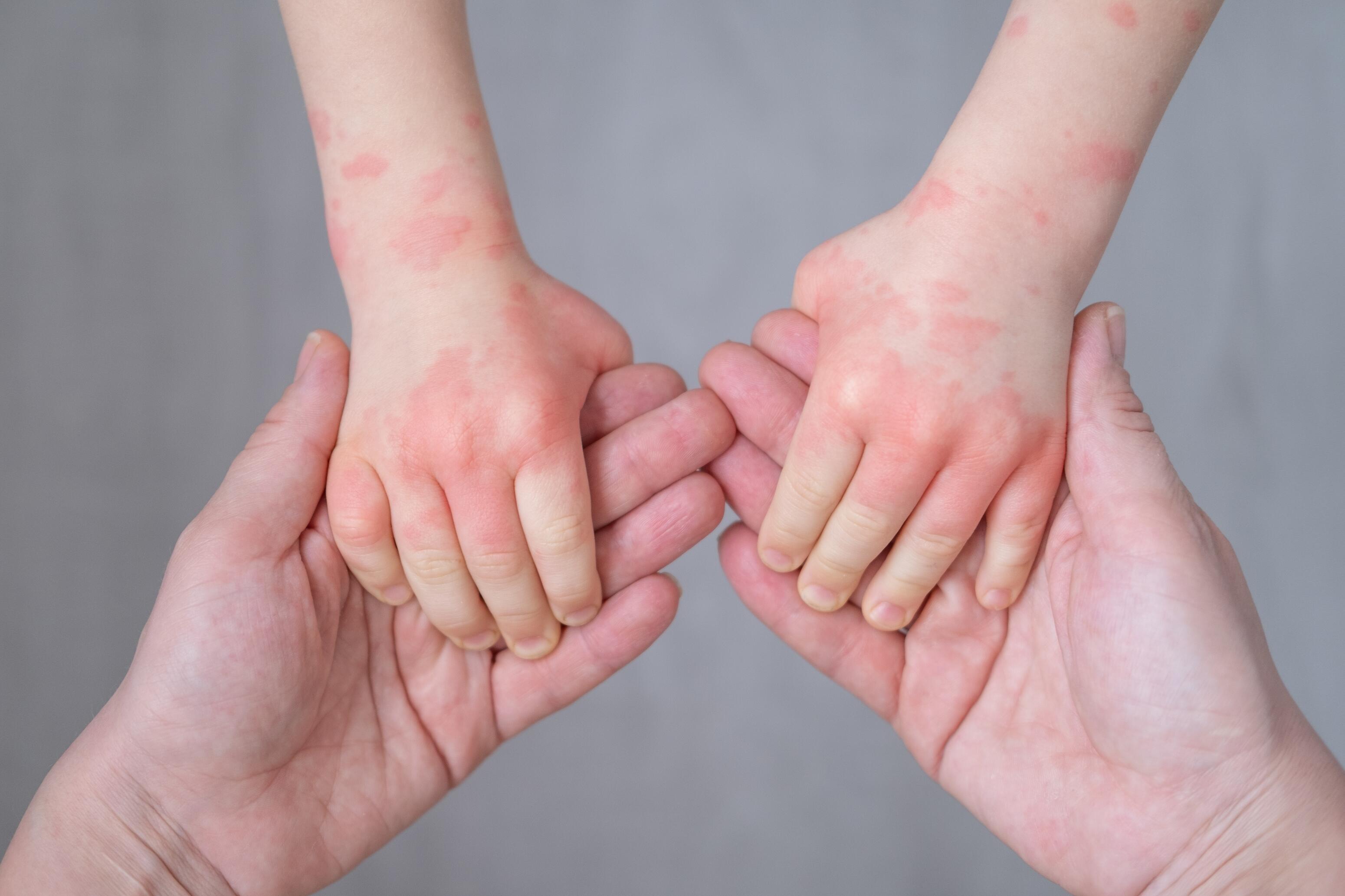
Atopic hand dermatitis usually begins in childhood and affects the back of the hands, wrists, palms, and spaces between the fingers.
This dermatitis, caused by protein exposure, starts with an urticaria-like eruption in the exposed areas and can then spread.
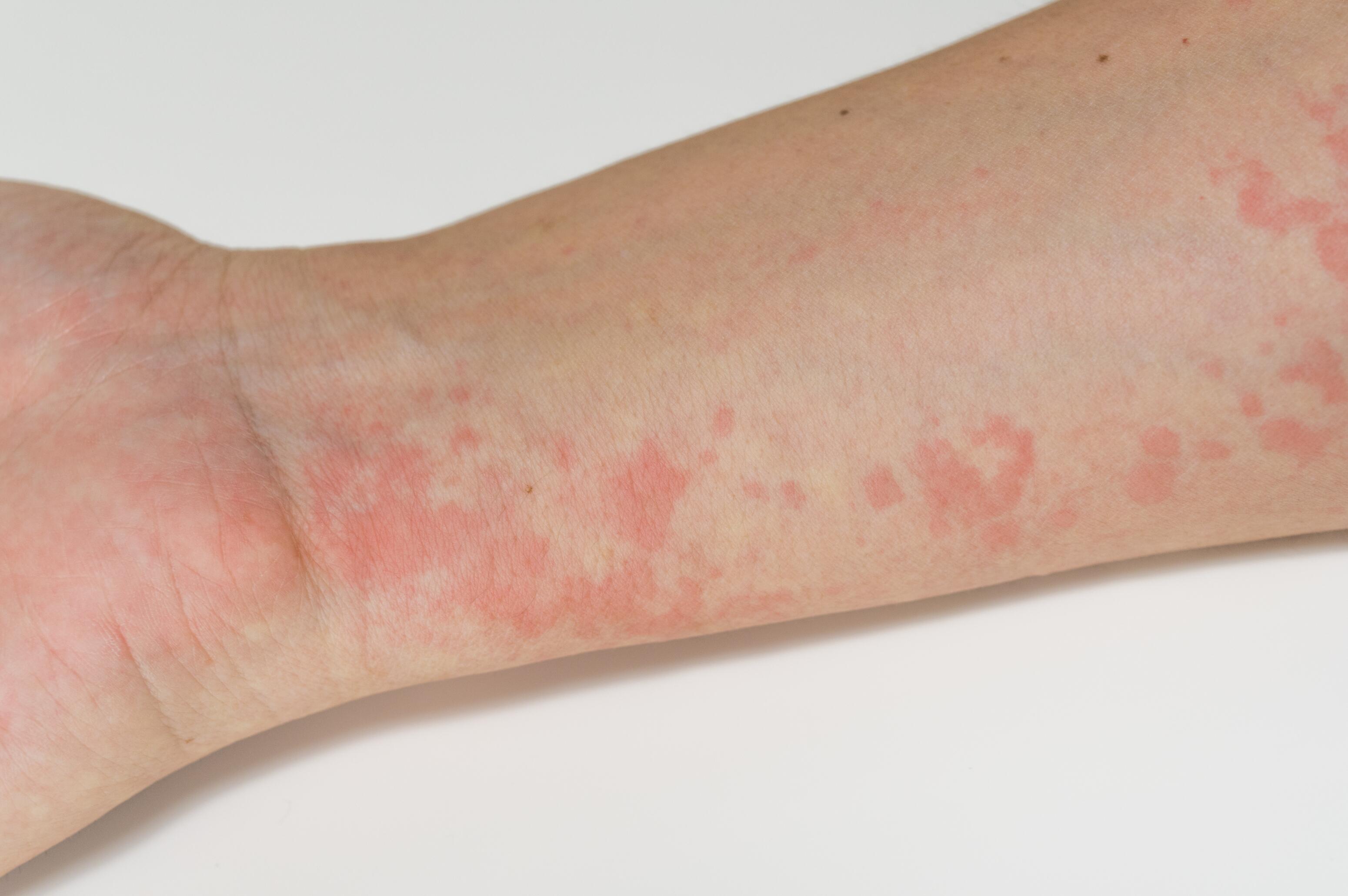
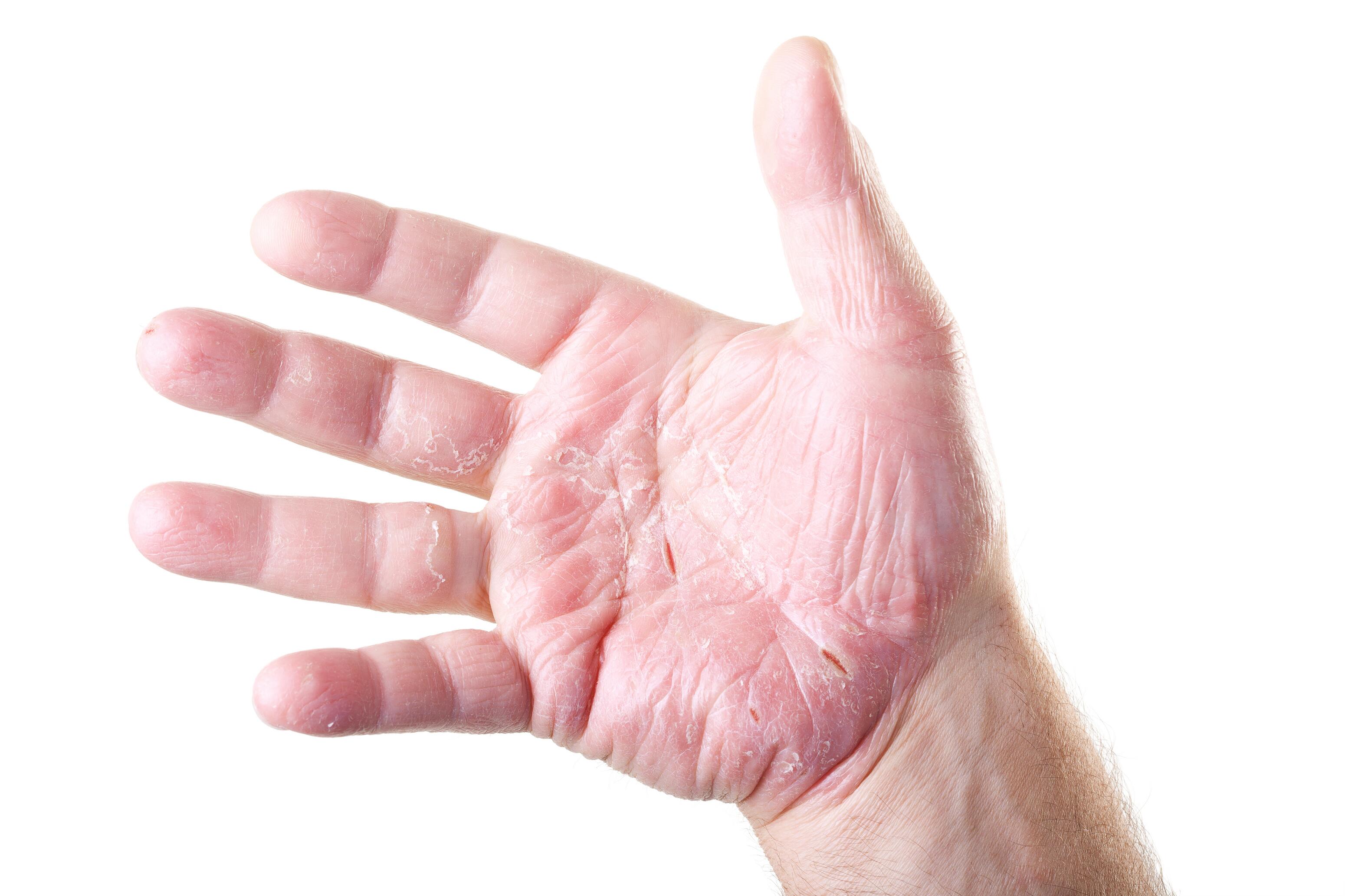
It is characterized by thickened skin, fissures, and pain, with mild itching. It mainly affects the palms.
Dyshidrosis is a type of eczema affecting the fingers and palms characterized by cyclical eruptions with numerous vesicles and significant itching.
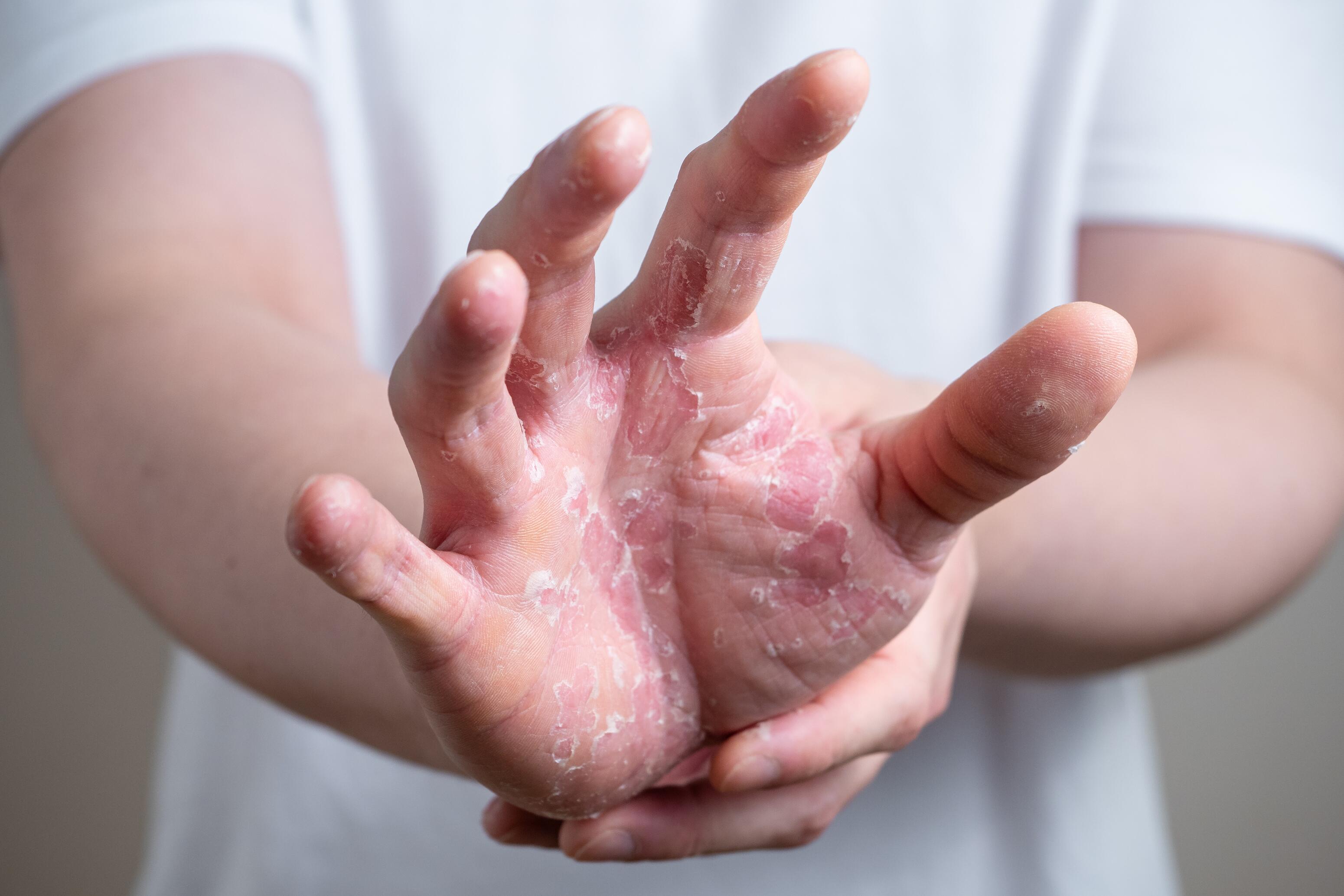

Often associated with atopic eczema, nummular dermatitis typically affects the back of the hands with dry skin and significant itching.
This dermatitis primarily affects the fingertips with thinned skin, pain, and minor itching.
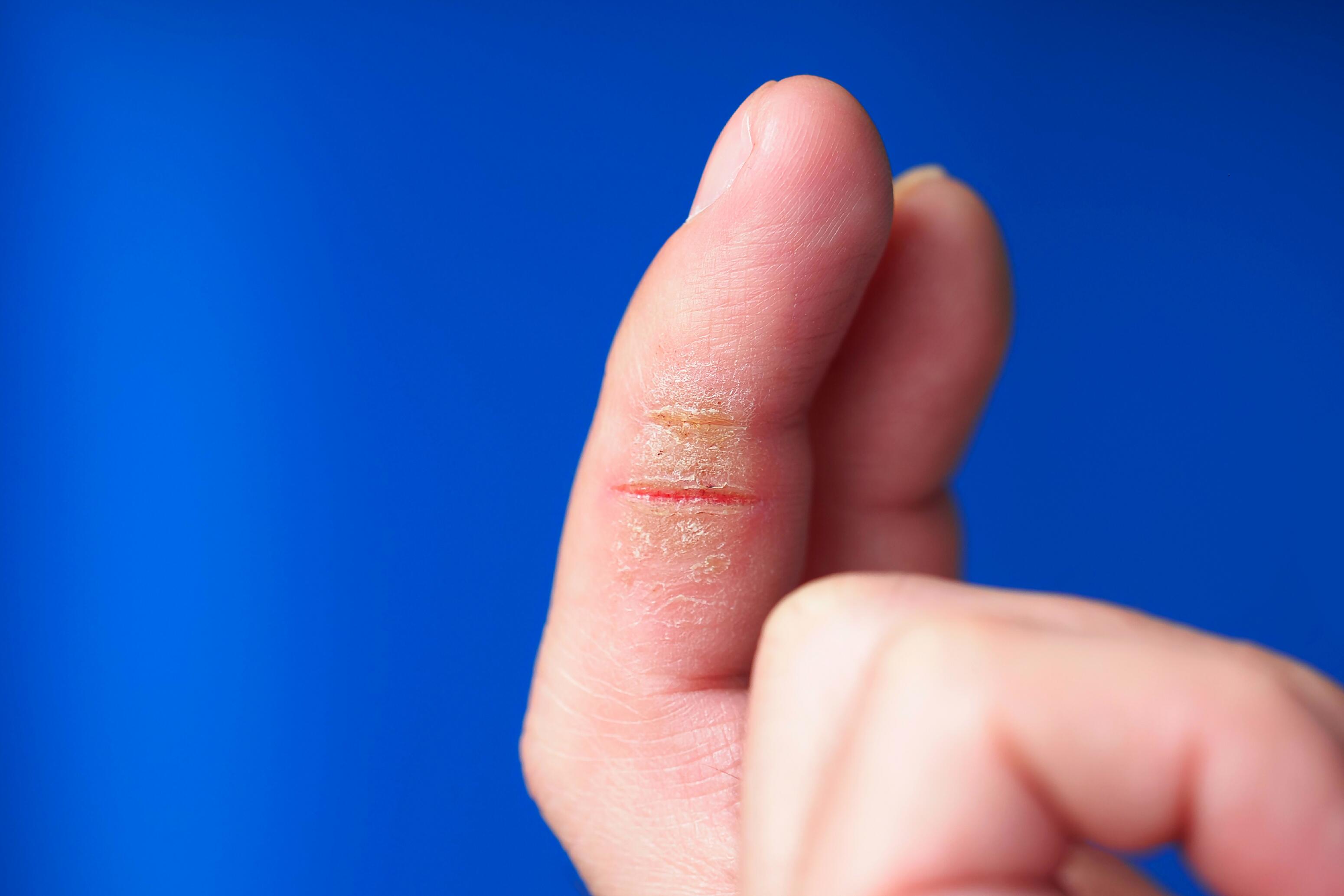
Treating hand dermatitis involves identifying and avoiding the environmental factors at play (allergens, irritants, proteins). The treatment must be adapted according to the disease's stage, causes, morphology, and locations. Eliminating emollients containing allergenic substances is essential.

Hydrating and caring for the skin with emollients helps to restore and maintain the skin barrier. The choice of emollient should consider individual preferences while avoiding allergens.
Corticosteroids, applied once a day, are the first short-term treatment for dermatitis. Intermittent long-term use can be considered for maintenance treatment.

Tacrolimus and/or pimecrolimus can be used in cases of topic corticosteroids' ineffectiveness or side effects (notably skin thinning).
Phototherapy can be used for adults with chronic dermatitis refractory to corticosteroids.
They are prescribed in some instances:
Daily management of hand dermatitis involves prevention measures, practical advice, and adapted skin care. Avoiding domestic and occupational environmental factors is the foundation of dermatitis prevention.
Prevention of hand dermatitis should thus begin at school, paying particular attention to children with atopic disorders, who are more likely to develop hand eczema later in life [3]
Occupational prevention in at-risk environments (hairdressers, caregivers, metalworkers, etc.) is crucial. It involves preventing irritant exposure, training for proper protective behavior, and using protective equipment. For example, avoid wearing rings if you work in wet conditions.
Here are some practical tips for handwashing, which are essential for removing harmful substances but can contribute to dermatitis if too frequent:
It is essential to use protective gloves for wet work and contact with irritants. Choose suitable gloves and keep them intact, clean, and dry inside. Glove usage should be limited in time to reduce the risks of irritative dermatitis due to friction and sweating.
Apply emollients several times daily to the whole hands, including the spaces between the fingers, the fingertips, and the backs. Use a fragrance-free, lipid-rich emollient cream for optimal hydration, especially before bedtime.
References:
1. Agner T, Elsner P. Hand eczema: epidemiology, prognosis and prevention. J Eur Acad Dermatol Venereol. 2020 Jan;34 Suppl 1:4-12.
2. Thyssen JP et al. Guidelines for diagnosis, prevention, and treatment of hand eczema. Contact Dermatitis. 2022 May;86(5):357-378.
3. Silvestre Salvador JF et al. Guidelines for the Diagnosis, Treatment, and Prevention of Hand Eczema. Actas Dermosifiliogr (Engl Ed). 2020 Jan 2;111(1):26-40.